6 results
Changing trends of suicide mortality from 2011 to 2019: an analysis of 38 European Countries
- G. Fico, A. Gimenez-Palomo, R. Andra Bursan, C. R. Ionescu, F. Kraxner, P. Rolland, S. Gomes-Rodrigues, M. Batković, E. Metaj, S. Tanyeri Kayahan, A. Mamikonyan, P. Paribello, A. K. Sikora, C. M. Platsa, M. Spasic Stojakovic, A. H. Halt, M. Az, N. Ovelian, K. Melamud, M. Janusz, K. Hinkov, C. Gramaglia, J. Beezhold, J. L. Castroman, C. Hanon, D. Eraslan, E. Olie
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S85-S86
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide is a serious public health problem since it accounts for nearly 900,000 deaths each year worldwide. Globally in 2019, 10.7 persons out of 100,000 died by suicide. Psychiatric disorders are related to an overwhelming proportion of these cases. In the last years, several specific interventions and action plans for suicide prevention have been implemented in a number of European countries.
ObjectivesOur aim was to analyze recent epidemiologic trends of suicide mortality rates in Europe.
MethodsAnnual national statistics of suicide mortality rates derived from Eurostat public databases from 2011 to 2019 were analyzed for 38 European countries. The suicide mortality rate was estimated per year/100,000 population. Linear regression models were used to study temporal trends of suicidal mortality. Analyses were performed using RStudio.
ResultsAvailable data show a statistically significant reduction in suicide mortality rates from 2011 to 2019 in 15 European countries, and a significant increase for Turkey (ES=0.32, SD=0.06, p=0.037) (Fig 1). The greatest significant decrease was reported in Lithuania (ES=-1.42, SD=0.02, p=0.02), followed by Hungary (ES=-1.13, SD=0.11, p=0.0007), Latvia (ES=-0.76, SD=0.11, p=0.007), and Poland (ES=-0.73, SD=0.10, p=0.001). Italy reported the lowest significant reduction in suicide mortality rates (ES=-0.13, SD=0.018, p=0.003). The remaining 16 countries showed no significant changes in suicide mortality trends.
Image:
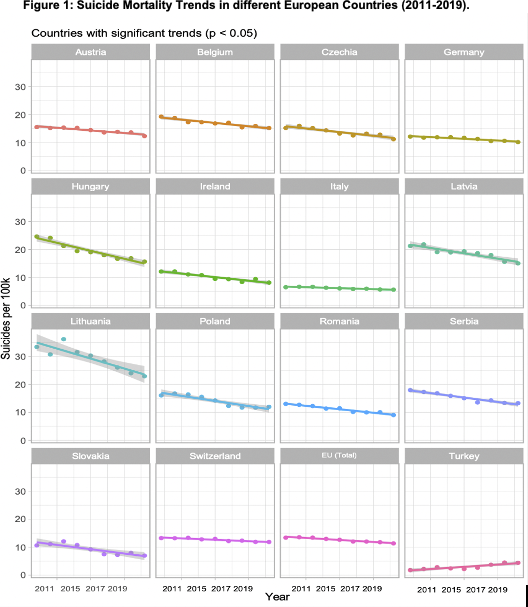 Conclusions
ConclusionsIn the last years, Europe registered an overall reduction in reported suicide rates. However, more recent data (i.e., suicide rates after COVID-19 pandemic, age and sex-related effect on suicide rates) should be analyzed and used to implement future recommendations. Current and future suicide prevention strategies aim to contribute to a greater reduction of suicide rates in the different European countries.
Disclosure of InterestNone Declared
Recovery from DSM-IV post-traumatic stress disorder in the WHO World Mental Health surveys
- A. J. Rosellini, H. Liu, M. V. Petukhova, N. A. Sampson, S. Aguilar-Gaxiola, J. Alonso, G. Borges, R. Bruffaerts, E. J. Bromet, G. de Girolamo, P. de Jonge, J. Fayyad, S. Florescu, O. Gureje, J. M. Haro, H. Hinkov, E. G. Karam, N. Kawakami, K. C. Koenen, S. Lee, J. P. Lépine, D. Levinson, F. Navarro-Mateu, B. D. Oladeji, S. O'Neill, B.-E. Pennell, M. Piazza, J. Posada-Villa, K. M. Scott, D. J. Stein, Y. Torres, M. C. Viana, A. M. Zaslavsky, R. C. Kessler
-
- Journal:
- Psychological Medicine / Volume 48 / Issue 3 / February 2018
- Published online by Cambridge University Press:
- 19 July 2017, pp. 437-450
-
- Article
- Export citation
-
Background
Research on post-traumatic stress disorder (PTSD) course finds a substantial proportion of cases remit within 6 months, a majority within 2 years, and a substantial minority persists for many years. Results are inconsistent about pre-trauma predictors.
MethodsThe WHO World Mental Health surveys assessed lifetime DSM-IV PTSD presence-course after one randomly-selected trauma, allowing retrospective estimates of PTSD duration. Prior traumas, childhood adversities (CAs), and other lifetime DSM-IV mental disorders were examined as predictors using discrete-time person-month survival analysis among the 1575 respondents with lifetime PTSD.
Results20%, 27%, and 50% of cases recovered within 3, 6, and 24 months and 77% within 10 years (the longest duration allowing stable estimates). Time-related recall bias was found largely for recoveries after 24 months. Recovery was weakly related to most trauma types other than very low [odds-ratio (OR) 0.2–0.3] early-recovery (within 24 months) associated with purposefully injuring/torturing/killing and witnessing atrocities and very low later-recovery (25+ months) associated with being kidnapped. The significant ORs for prior traumas, CAs, and mental disorders were generally inconsistent between early- and later-recovery models. Cross-validated versions of final models nonetheless discriminated significantly between the 50% of respondents with highest and lowest predicted probabilities of both early-recovery (66–55% v. 43%) and later-recovery (75–68% v. 39%).
ConclusionsWe found PTSD recovery trajectories similar to those in previous studies. The weak associations of pre-trauma factors with recovery, also consistent with previous studies, presumably are due to stronger influences of post-trauma factors.
The cross-national epidemiology of DSM-IV intermittent explosive disorder
- K. M. Scott, C. C. W. Lim, I. Hwang, T. Adamowski, A. Al-Hamzawi, E. Bromet, B. Bunting, M. P. Ferrand, S. Florescu, O. Gureje, H. Hinkov, C. Hu, E. Karam, S. Lee, J. Posada-Villa, D. Stein, H. Tachimori, M. C. Viana, M. Xavier, R. C. Kessler
-
- Journal:
- Psychological Medicine / Volume 46 / Issue 15 / November 2016
- Published online by Cambridge University Press:
- 30 August 2016, pp. 3161-3172
-
- Article
- Export citation
-
Background
This is the first cross-national study of intermittent explosive disorder (IED).
MethodA total of 17 face-to-face cross-sectional household surveys of adults were conducted in 16 countries (n = 88 063) as part of the World Mental Health Surveys initiative. The World Health Organization Composite International Diagnostic Interview (CIDI 3.0) assessed DSM-IV IED, using a conservative definition.
ResultsLifetime prevalence of IED ranged across countries from 0.1 to 2.7% with a weighted average of 0.8%; 0.4 and 0.3% met criteria for 12-month and 30-day prevalence, respectively. Sociodemographic correlates of lifetime risk of IED were being male, young, unemployed, divorced or separated, and having less education. The median age of onset of IED was 17 years with an interquartile range across countries of 13–23 years. The vast majority (81.7%) of those with lifetime IED met criteria for at least one other lifetime disorder; co-morbidity was highest with alcohol abuse and depression. Of those with 12-month IED, 39% reported severe impairment in at least one domain, most commonly social or relationship functioning. Prior traumatic experiences involving physical (non-combat) or sexual violence were associated with increased risk of IED onset.
ConclusionsConservatively defined, IED is a low prevalence disorder but this belies the true societal costs of IED in terms of the effects of explosive anger attacks on families and relationships. IED is more common among males, the young, the socially disadvantaged and among those with prior exposure to violence, especially in childhood.
Barriers to mental health treatment: results from the WHO World Mental Health surveys
- L. H. Andrade, J. Alonso, Z. Mneimneh, J. E. Wells, A. Al-Hamzawi, G. Borges, E. Bromet, R. Bruffaerts, G. de Girolamo, R. de Graaf, S. Florescu, O. Gureje, H. R. Hinkov, C. Hu, Y. Huang, I. Hwang, R. Jin, E. G. Karam, V. Kovess-Masfety, D. Levinson, H. Matschinger, S. O'Neill, J. Posada-Villa, R. Sagar, N. A. Sampson, C. Sasu, D. J. Stein, T. Takeshima, M. C. Viana, M. Xavier, R. C. Kessler
-
- Journal:
- Psychological Medicine / Volume 44 / Issue 6 / April 2014
- Published online by Cambridge University Press:
- 09 August 2013, pp. 1303-1317
-
- Article
- Export citation
-
Background
To examine barriers to initiation and continuation of mental health treatment among individuals with common mental disorders.
MethodData were from the World Health Organization (WHO) World Mental Health (WMH) surveys. Representative household samples were interviewed face to face in 24 countries. Reasons to initiate and continue treatment were examined in a subsample (n = 636 78) and analyzed at different levels of clinical severity.
ResultsAmong those with a DSM-IV disorder in the past 12 months, low perceived need was the most common reason for not initiating treatment and more common among moderate and mild than severe cases. Women and younger people with disorders were more likely to recognize a need for treatment. A desire to handle the problem on one's own was the most common barrier among respondents with a disorder who perceived a need for treatment (63.8%). Attitudinal barriers were much more important than structural barriers to both initiating and continuing treatment. However, attitudinal barriers dominated for mild-moderate cases and structural barriers for severe cases. Perceived ineffectiveness of treatment was the most commonly reported reason for treatment drop-out (39.3%), followed by negative experiences with treatment providers (26.9% of respondents with severe disorders).
ConclusionsLow perceived need and attitudinal barriers are the major barriers to seeking and staying in treatment among individuals with common mental disorders worldwide. Apart from targeting structural barriers, mainly in countries with poor resources, increasing population mental health literacy is an important endeavor worldwide.
Mood and anxiety disorders across the adult lifespan: a European perspective
- R. D. McDowell, A. Ryan, B. P. Bunting, S. M. O'Neill, J. Alonso, R. Bruffaerts, R. de Graaf, S. Florescu, G. Vilagut, J. M. C. de Almeida, G. de Girolamo, J. M. Haro, H. Hinkov, V. Kovess-Masfety, H. Matschinger, T. Tomov
-
- Journal:
- Psychological Medicine / Volume 44 / Issue 4 / March 2014
- Published online by Cambridge University Press:
- 31 May 2013, pp. 707-722
-
- Article
- Export citation
-
Background
The World Mental Health Survey Initiative (WMHSI) has advanced our understanding of mental disorders by providing data suitable for analysis across many countries. However, these data have not yet been fully explored from a cross-national lifespan perspective. In particular, there is a shortage of research on the relationship between mood and anxiety disorders and age across countries. In this study we used multigroup methods to model the distribution of 12-month DSM-IV/CIDI mood and anxiety disorders across the adult lifespan in relation to determinants of mental health in 10 European Union (EU) countries.
MethodLogistic regression was used to model the odds of any mood or any anxiety disorder as a function of age, gender, marital status, urbanicity and employment using a multigroup approach (n = 35500). This allowed for the testing of specific lifespan hypotheses across participating countries.
ResultsNo simple geographical pattern exists with which to describe the relationship between 12-month prevalence of mood and anxiety disorders and age. Of the adults sampled, very few aged ⩾80 years met DSM-IV diagnostic criteria for these disorders. The associations between these disorders and key sociodemographic variables were relatively homogeneous across countries after adjusting for age.
ConclusionsFurther research is required to confirm that there are indeed stages in the lifespan where the reported prevalence of mental disorders is low, such as among younger adults in the East and older adults in the West. This project illustrates the difficulties in conducting research among different age groups simultaneously.
Cross-national differences in the prevalence and correlates of burden among older family caregivers in the World Health Organization World Mental Health (WMH) Surveys
- V. Shahly, S. Chatterji, M. J. Gruber, A. Al-Hamzawi, J. Alonso, L. H. Andrade, M. C. Angermeyer, R. Bruffaerts, B. Bunting, J. M. Caldas-de-Almeida, G. de Girolamo, P. de Jonge, S. Florescu, O. Gureje, J. M. Haro, H. R. Hinkov, C. Hu, E. G. Karam, J.-P. Lépine, D. Levinson, M. E. Medina-Mora, J. Posada-Villa, N. A. Sampson, J. K. Trivedi, M. C. Viana, R. C. Kessler
-
- Journal:
- Psychological Medicine / Volume 43 / Issue 4 / April 2013
- Published online by Cambridge University Press:
- 09 August 2012, pp. 865-879
-
- Article
- Export citation
-
Background
Current trends in population aging affect both recipients and providers of informal family caregiving, as the pool of family caregivers is shrinking while demand is increasing. Epidemiological research has not yet examined the implications of these trends for burdens experienced by aging family caregivers.
MethodCross-sectional community surveys in 20 countries asked 13 892 respondents aged 50+ years about the objective (time, financial) and subjective (distress, embarrassment) burdens they experience in providing care to first-degree relatives with 12 broadly defined serious physical and mental conditions. Differential burden was examined by country income category, kinship status and type of condition.
ResultsAmong the 26.9–42.5% respondents in high-, upper-middle-, and low-/lower-middle-income countries reporting serious relative health conditions, 35.7–42.5% reported burden. Of those, 25.2–29.0% spent time and 13.5–19.4% money, while 24.4–30.6% felt distress and 6.4–21.7% embarrassment. Mean caregiving hours per week in those giving any time were 16.6–23.6 (169.9–205.8 h/week per 100 people aged 50+ years). Burden in low-/lower-middle-income countries was 2- to 3-fold higher than in higher-income countries, with any financial burden averaging 14.3% of median family income in high-, 17.7% in upper-middle-, and 39.8% in low-/lower-middle-income countries. Higher burden was reported by women than men and for conditions of spouses and children than parents or siblings.
ConclusionsUncompensated family caregiving is an important societal asset that offsets rising formal healthcare costs. However, the substantial burdens experienced by aging caregivers across multiple family health conditions and geographic regions threaten the continued integrity of their caregiving capacity. Initiatives supporting older family caregivers are consequently needed, especially in low-/lower-middle-income countries.




